Treating arrhythmia with radiation yields healthier heart tissue, researchers say
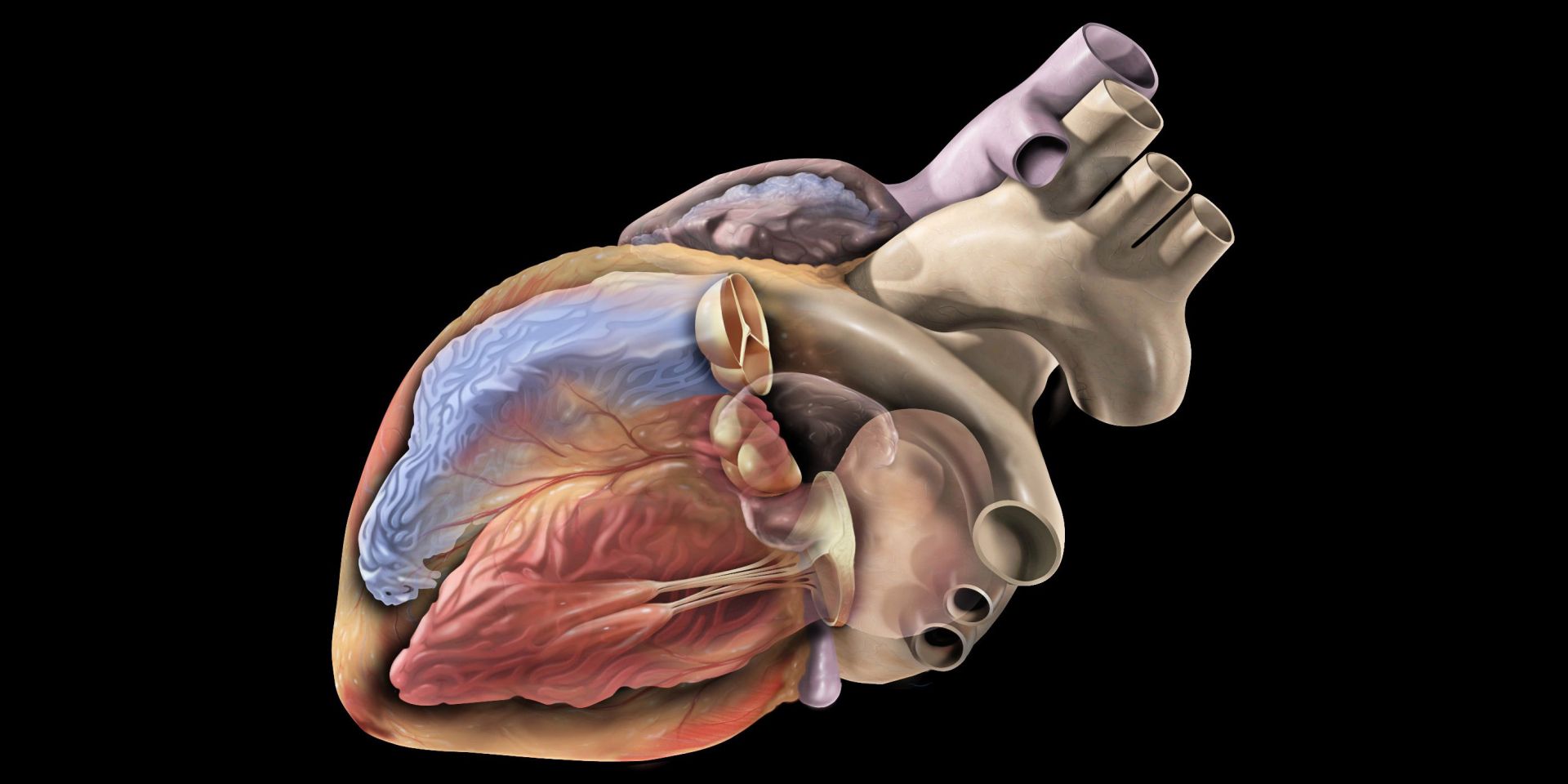
Therapeutic radiation is typically reserved for cancer treatment, but scientists at Washington University School of Medicine in St. Louis have applied radiation therapy to treat ventricular tachycardia, a life-threatening heart arrhythmia. A news release issued by the university says that the results of the study show that radiation therapy can “reprogram” heart muscle cells to “a younger and perhaps healthier state.” The findings were published in the journal Nature Communications on September 24.